Two years after the military defeat of ISIS in Northern Iraq, traumas of the terror years rise to the surface on a scale that far overstretches the health system. This is why Cordaid has scaled up its mental health services and psychosocial support in different locations. The needs are overwhelming, as a journey to several health facilities shows.

The health system in Iraq is facing major challenges and gaps due to local humanitarian and economic crises. All healthcare services are overloaded: their capacity is exhausted, and there is a huge and immediate need to provide essential life-saving services. Since 2017, Cordaid has supported basic healthcare services in North Iraq for the most vulnerable populations, such as returned minorities, internally displaced people, and host communities, encouraging safe and voluntary return.
Sinjar Hospital, on any weekday, is a crowded place. Especially on the first floor, where Cordaid runs a mental health and psychosocial support (MHPSS) department. Especially this day, when the psychiatrist organizes a weekly group session and has individual consultations. Several psychosocial workers assist him. Suddenly, in the busy hallway, one of the patients collapses. In no time, she is gently and professionally assisted by one of the social workers. And by another patient. “She relives the nightmare”, explains one of the staff as the collapsed woman is being assisted. “We see this a lot.”
“A lot of people say ISIS is still there, under the radar, in sleeping cells, biding their time. Hence, the checkpoints. And the unwillingness to return.”
So far, only 6000 people have returned to Sinjar. This Yazidi ‘capital’ in Ninewa province, close to Syria, used to have more than 80,000 inhabitants. ISIS attacked and took the town in August 2014, only to be expelled in November 2015 by Kurdish forces. 15 months of utter horror.
Setting Up a Mental Health Department in Former ISIS Territory
The number of returnees may be small, but all are scarred for life and need whatever support they can get. Yet the whole province of Ninewa, with its millions of inhabitants, has no more than a handful of psychiatrists. No wonder people are queuing for Dr. Muhazim Muhammed, the department’s psychiatrist.

“This department is the only facility that provides mental health care and psychosocial support at the hospital level in the whole of Sinjar”, explains Hala Saba Jameel, who coordinates Cordaid’s health program in Iraq. “We trained social workers and mobile teams, especially in recognizing and addressing gender-based violence. We pay their salaries, provide the equipment, and offer incentives to the psychiatrist. The mobile staff goes out to the surrounding villages daily, talks to the families tries to find those most urgently in need of support and informs them of our psychosocial and mental health care activities. We ensure there’s always someone there for them to listen to them and provide professional care. The department has been up and running for 5 months.”
“We slept in a mountain shed. There was no food, no water. One moment, ISIS was near; they saw us and shot at us. We escaped.”
ISIS rule and the ensuing war traumatised all communities in Iraq, whether Shia, Sunni, Kurdish, Christian or other groups. Nevertheless, the extent of targeted and organized brutalities against the Yazidis is unprecedented. Yazidi history knows many persecutions. This one stands out. Thousands of women and girls were raped, kidnapped, enslaved and sold. Thousands of men and boys were killed. So far, over 70 mass graves in and around Sinjar have been unearthed.
Fear Never Left the Area
It is reckoned that of the 550,000 Yazidis in Northern Iraq, 100,000 have fled abroad, 350,000 still live a life in limbo in IDP camps, and many thousands sought refuge with relatives or in unfinished houses. 3000 people are still missing. To survive as a people, the Yazidi pray, sing and gather in their temples and other places of worship. They adapt age-old baptism rituals to ‘cleanse’ ISIS rape victims of stigma and shame and to welcome them back into the closed Yazidi community. It is not enough to heal wounds. Nothing ever is.
ISIS’ evil nature is still omnipresent wherever you go in this part of Iraq. It’s in the faces, hearts and souls of their survivors. It’s in the black graffiti on the ruins of the houses they occupied. It’s in the iron sniper cages hidden in trees, not yet dismantled, years after they left. A lot of people say ISIS is still there, under the radar, in sleeping cells, biding their time. Fear never left this area. Hence, the checkpoints. And the unwillingness to return.
“I am 52 years old, and I have never seen trauma on this scale.”
One of the more gruesome illustrations of evil is the story of Sinjar’s old hospital. It’s in the heart of the ghost part of town, a landscape of ruins. “ISIS turned this hospital into their rape centre”, says Cordaid’s Hala Saba Jameel. “Today, people do not wish to go there, even though it has been rehabilitated and partly functioning. That’s why health authorities turned a primary health centre in another part of town into a hospital. That’s where we decided to have our MHPSS department”, she explains.
Baran Omer is one of the regular patients at the MHPSS department in the new Sinjar hospital. Her story is one among many. She and her family fled on the sinister day ISIS fighters took the town of Sinjar on August 3, 2014. “Like the others, we walked towards the mountain”, she recalls. Of the ones that stayed behind, some of them Baran’s relatives, many were killed. “For a couple of days, we kept together as a family. We slept in a mountain shed. There was no food, no water. One moment, ISIS was near, saw us and shot at us. We escaped”, Baran continues. “My husband and some of our children moved fast. At one point, I lagged behind as I carried my teenage daughter. She has been paralysed since birth. She also has mental problems and needs special, liquid food. Only I could take care of her. I told my husband to move on with the other children. Me and my daughter were too exhausted. We decided to hide under an abandoned tractor.”
Soon after, Baran and her daughter are caught and taken away by ISIS, together with other women and children. “Before they locked us up, they executed eight men right in front of us.”

“We were kept inside a room. The first days, we were beaten and flogged. I did my utmost to feed my daughter. Often they came to rape me, but each time I cried and begged them not to, explaining the hardship of my daughter. This worked for a while. Until that evening, after 13 days. I knew they were going to rape me. Somehow, I managed to run away back to the mountain. I had to leave my daughter behind. It was horrible. I could not think any longer. I ran the whole night and saw a lot of dead bodies. I was like an animal. I didn’t feel anything. I ate the leaves from the trees.”
Baran survives. She even manages to join her husband and other children. But up to today, she hasn’t heard about the daughter she had carried up the mountain and cared for in captivity five years ago. She received a letter from the Iraqi authorities telling her they presumed her daughter had died.
Today, Baran receives psychosocial support and psychiatric treatment. “Medication helps me to live”, she says. “And to work. My husband is diabetic and has no job.”
Every Survivor Needs Treatment
As the psychiatrist Dr Muhazim Muhammed explains, every single survivor requires treatment. But with so few psychiatrists and psychotherapists around, only a few can get it. “Being kidnapped, having a family that is or was kidnapped, being raped or abused, losing your house, losing a family member… These are all deeply traumatising experiences”, says Dr Muhammed. “I am 52 years old, and I have never seen trauma on this scale.”
Luckily, the Sinjar MHPSS department manages to provide psychotropic medication for free. So far, with Cordaid support, they have not run out of stock. With all the checkpoints in this part of Iraq and safety procedures changing daily, this is a logistical and administrative triumph.
“We couldn’t wash ourselves, we were beaten constantly. In the presence of all the others. My kids saw a lot of things. They still have nightmares.”
Not being able to do enough is the most frustrating feeling for all health professionals. “In times of crisis, we work with whatever we have”, says Dr Muhammed. “All patients are being taken care of by our nurses. Some are then referred to our psychosocial workers for extra support. The most severe cases, the ones who are suicidal and the ones with severe mental disorders, are treated by me individually. But the reality is that we should do a lot more than we are doing now.”

In the Sinjar hospital entrance hall, some kids are having fun in a small playground under the caring attention of a Cordaid social worker. Their mother came to the hospital to meet the psychiatrist. She has a harrowing tale to tell but doesn’t want her name or her picture to be published. Like so many, she carries a weight no one should be forced to carry.
Escaping ISIS
The day ISIS came, she and her three youngest kids were dragged out of the house and taken away. At that time, her husband was at the market. Like cattle, they were being moved from place to place and lived in makeshift prisons for months. “Now and again, fighters came and raped the most beautiful girls”, she says. “After a while, they also took the older women.”
This is how they survive for a year: she and her kids, the youngest at the time, are a year old. “We only had rice, water and bread. We couldn’t wash, and we were beaten constantly. In the presence of all the others. My kids saw a lot of things. They still have nightmares.”
Once, she and a few other mothers try to escape. They fail. “We were beaten badly.” They try a second time, showing amazing courage and cunning. “One of the girls had a mobile hidden in a sock. She called a man she knew outside. He was ready to pick us up with a van at a certain time and place – the nearest hospital. He also told us how to escape.”

So, one night, six mothers and their children wear whatever black clothes they can find. It’s the best ISIS outfit they can think of. At one point, in the dead of night, the door of their prison stays open for a short while. They sneak out in silence. And make it to the hospital, where a van is signalling with its headlights. Off they go, 20 km to the nearest Kurdish peshmerga checkpoint. They make it, and they are alive. Each of these mothers’ relatives had paid the driver 15,000 US dollars. It was the price he had asked.
Years later, she and her family keep on paying for what happened. “My kids have lost years of school. They are depressed, like me”, says the mother. “Myself, I keep having these epileptic fits. I have bad dreams; I am full of fear and anger. My husband is thankful that we are all together. But he is frustrated. Full of things inside. Much angrier than he was when we first met. People tell me to look ahead. I can’t. I can only look back.”
The family used to live in the centre of Sinjar. “We decided to go back to Sinjar. But since our house in the centre was destroyed, we now live in a suburb, in a house that was only partly burnt down. Now and again, my husband has odd jobs in building and construction. It’s hardly enough to make ends meet.”
Mornings are the worst. “My three youngest go to school”, the mother says. “It’s an hour’s walk to get there. Every time I watch them go, I am terrified that I will never see them again. Without the psychiatrist, the mental support and the medication, I would not be able to keep on going the way I do.”
Heavily Armed Checkpoints
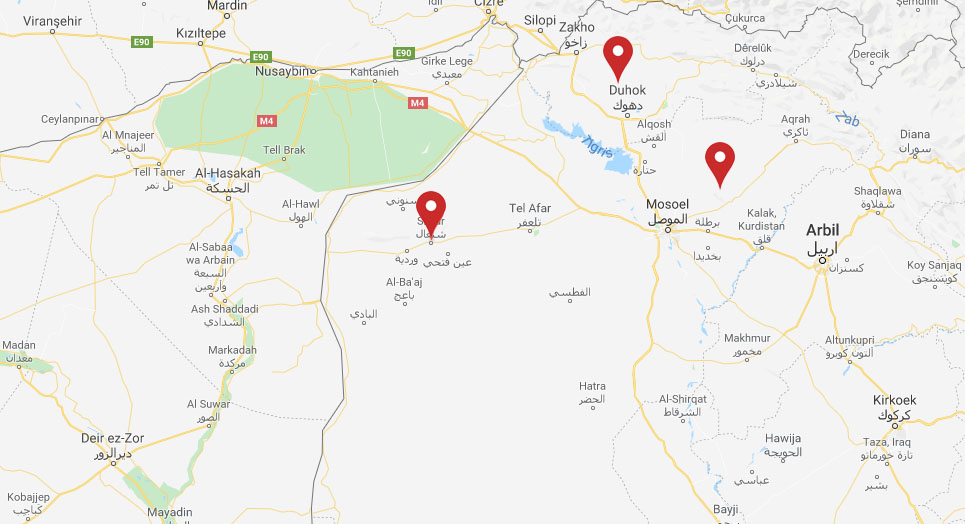
Some 200 kilometres to the east, following a string of heavily armed checkpoints and passing several IDP camps under a blazing sun, lies the town of Ba’ashiqa. It used to be known as a place where Muslim, Christian and Yazidi communities lived side by side in peace.
Amar Qassar, a pharmacist and part of the Cordaid health team in Iraq, grew up in Mosul. He guesses that about half of Ba’ashiqa’s population has returned. “Before ISIS got here, everybody had left the place”, he says.
One of the reasons for people to return and to stay – apart from basic safety, housing, job opportunities and schooling for kids – is the presence of healthcare facilities. “There were none here”, Amar explains. “ISIS looted and destroyed all facilities before they were pushed out”, he explains.
In the past year, Cordaid staff in Iraq rehabilitated four basic but essential health facilities in the rural outskirts of Ba’ashiqa. All of the ‘health houses’ are located near a school and near or inside a village. “They are smaller than the primary health care centre in town. Cordaid wanted to restore them because so many people can’t afford transportation to the centre. And sometimes, in urgent cases, it takes too long to get there. And by revitalizing these rural health facilities, we unclog overburdened health services inside the town”, Amar explains.
Turning Empty Lots into Health Facilities
Cordaid staff purchased prefab housing units—several for each health facility—generators and medical equipment. We supply essential drugs. We pay the salaries of the nurses, pharmacist assistants, and social workers who run the facilities and treat the patients—more than 30 on average a day. We pay an incentive for the psychiatrist who visits the health houses once a week.
So, in a couple of months, four empty lots were turned into primary health and mental health units people can rely on. They are essential because apart from dealing with a post-war situation—fear, sectarian tensions, damaged houses, and joblessness—people have to deal with daily life, with common things like diarrhoea, diabetes, infections, hypertension, and depression.
“Only last week, we saved a baby’s life. It had an acute chest infection. Luckily, we had a vaporizer and the right drugs”, says the nurse in the health house of Baybokht village. Like all staff, he was displaced for years. “I returned from the south after ISIS was driven away and the electricity was re-installed in this area.”
Struggle within a Struggle: Women’s Fight for Freedom and Basic Rights
Hanin Rafa is the social worker in Baybokht. She’s a young woman who – despite the war and with an interval of several years – graduated in psychology at Mosul University. She does what all Cordaid-supported social workers do. “I want girls and women here to stand up for themselves”, she explains. “It’s very delicate. Most women are not allowed to go out of the house. If they do, sometimes their husbands want to divorce. They have no rights at all. They are stuck. At least 50% of them cannot read and write”, she says. On top of the big war and ISIS rule that all of them have survived, women, especially in the more conservative rural areas, have another battle to fight for: the one for freedom and basic rights. The one against domestic restraint and violence.
Hanin’s work, like any trust-building work, asks for patience. “The first step is to invite them to come to my sessions. If one woman comes, others may follow more easily. I encourage them to discuss things with their husbands. And here, in my separate room in the health facility, we do several things. I teach them to read and write. That opens a world. We talk about the problems they have and how to overcome them. They support each other. Some girls drop out, some stay.”
10 km down the dusty road, at the health house in Dar Awash village, women and kids have come in such numbers they almost block the entrance. Wasila Mohammad, a Muslim mother who lives nearby, is one of them. “It’s good this place has reopened. We come here often, including my six children and me. It’s too expensive to go to the health centre in Ba’ashiqa town”, she says. “When I was bitten by a snake while working in the field, I ran to this place”, says Ghazal Brahim. “They took out the venom and gave me the right drugs.” Another young woman, Sosen Ali, would like the health centre to have a gynaecologist. “For 10 years, I’ve been trying to have a child. I can’t afford to go to a hospital for a sonar check. I wish they could help me here”, she says.

All the women and their kids are waiting for the group session with the psychosocial worker. It has started recently. “We come here to clear our hearts and to learn new things. Like sewing, making clothes, and reading. Soon, we can sell the things we make”, Sosen says. “We feel lighter after the sessions. And we know more. We are less afraid to share our psychological problems. Even with the psychiatrist, who comes here once a week”, says another woman. “If only they had this for men too. It would help them to vent their frustrations. To be more open and less violent”, she continues.
So eager are women to come to the sessions—with their smaller kids at their side—that new problems arise. “The room is too crowded, too small, and too hot,” Sosen says. A facility nurse explains that this is why they are thinking of creating a separate and safe playground for the children on the small compound.
Mechanic, Farmer, and Mother
Wasila shares part of her story. She spent a few years in an IDP camp after ISIS took her village and occupied her house. “We fled in time. We ended up in an IDP camp in the Kurdistan Region. Life there was hard. The heat and cold were unbearable.”

Like others, Wasila decided to come back once she knew Iraqi militias had come back to Ba’ashiqa. “Our house was partly damaged. And the water well was destroyed. Still, life here is better than inside the camps”, she says. Her husband is jobless. He used to be a truck driver but lost an arm in an accident. Now, it’s Wasila who raises an income. She sells the vegetables she grows herself. And she works as a mechanic. “I repair generators and water pumps in the village.” Wasila is still angry when she shows the damage ISIS did to her house years ago. “If they ever return, I will defend my house. I am stronger than my husband. With one ar,m he cannot fight.”
Seje
We leave Ba’ashiqa. We cross the river Tigris, leave the Ninewa Plains and pass the heavily guarded border with the Kurdistan Region in Iraq. This autonomous part of Iraq was never invaded by ISIS, thanks to fierce resistance by Kurdish fighters, the Peshmerga. Here, in the Christian village of Seje, near the city of Dohuk, Cordaid decided to start its healthcare intervention at a time when the war with ISIS was still undecided more than two years ago. “This was the right spot to start”, says Albert van Hal, Cordaid’s Health program manager based in The Hague. “At the time, we couldn’t enter Ninewa province because of the war. Kurdistan welcomed hundreds of thousands of IDPs back then. Most of them are still waiting to go back. Many reside in camps. Some stay in unfinished houses inside and around villages like Seje. So we decided to expand, re-equip and re-staff a very basic health centre in Seje, in collaboration with the Dohuk District of Health. Not only to provide health care for the displaced, mostly Yazidi families. Also for the host communities who were outnumbered and could hardly cope with the situation”, van Hal continues. “The idea was that if we do well in Seje, we can later expand to other locations.”

Two years later, the primary health care centre of Seje is the main health facility for many miles around. It has a doctor’s room; two nurses have their unit; there’s a pharmacy, clean toilets, a waiting room, and a room for psychosocial support. “All chronic and common diseases are treated here”, says Amar Qasar from Cordaid. “Unfortunately, we do not have the means for an emergency room and a maternity ward. We provide first aid care, but people must go to Dohuk Hospital for serious injuries or emergencies, which is half an hour’s drive. Sometimes, if people cannot pay for transportation, we use the Cordaid vehicle as an ambulance. Recently, we did this for an older man who was in shock. And for a woman who was about to give birth”, Amar continues.
Mobile Clinics
From morning till afternoon, Seje Health Centre receives patients from Seje and the surrounding villages. Half of them are displaced Yazidi people; half are residents. “The Seje centre also has a well-equipped and staffed mobile clinic”, Amar Qasar explains. “The Cordaid vehicle is packed with medical equipment and drugs. Every day, the driver, pharmacist and doctor visit families in the surrounding villages.”
About a year ago, Cordaid decided to add mental health and psychosocial support to its project in Seje. Months before Sinjar and Ba’ashiqa, this is where we started our MHPSS program. “The reason was simple”, says Hala Saba Jameel. “During and immediately after the war, the focus was on emergency health care. On survival. After people had escaped ISIS, joined their families, had found some sort of shelter, their traumas came to the surface. Issues of mental health and post-traumatic disorders became much more prominent. That is why Cordaid decided to recruit and train a psychosocial worker. For a year now, she has been part of Seje’s team. We also did our utmost to add a psychiatrist to the team. As you know, they are hard to find in Iraq.”
Tahireh Sadiq, the psychiatrist, visits the Seje health centre twice a month. It’s only one of the locations where she treats patients.
Psychiatrist and Social Worker Team Up
“Currently, I have about 15 patients in Seje, all women from Sinjar. They all have trauma-related disorders. Sonita Khalil, the Cordaid social worker at the centre, referred them to me. We work well together. We exchange files, discuss cases and decide how I, as a psychiatrist, and she, as a social worker, can best treat and support women. Sonita provides psychosocial care to Yazidi IDPs, mainly women and girls. As a young Yazidi woman herself, she knows their world and speaks their language. She does a terrific job”, Dr Sadiq explains.

“Displacement is a hugely traumatic experience. It deteriorates and aggravates any existing mental issue or disorder and can cause new ones. The ISIS crisis itself, even before people ended up being displaced, caused a massive peak in sleeping, eating and other disorders. Displacement and the bad socio-economic conditions that come with it cause new forms of suffering. The stress and poverty, on top of the loss of relatives and loss of homes, cause extra anxiety and more domestic violence. In a way, the suffering of displaced people increases with the years. After years of continuous trauma, treatment not only becomes more urgent but also more difficult.”
According to Dr Sadiq, the scope of mental needs and suffering is far bigger than health data can even start to depict. “Until now, no proper mental health assessments have been done in the whole of Northern Iraq. We know that every single person who was attacked and displaced by ISIS has had at least one and probably several deeply traumatic experiences. All of them need to be assessed and given the care they need. This takes time and a lot of patience. Traumatised persons, especially kids and adolescents, tend to become silent and withdrawn. Their signs of suffering and mental disorder are often not obvious. Only if we go from house to house, from camp to camp, and properly assess each person will we know the extent and the vastness of mental suffering caused by ISIS and the violent events”, says Dr Sadiq.
Mental Health Gap
Given this scale of suffering, the lack of psychiatrists in Iraq is staggering. But there’s more than that, according to Dr Sadiq. “Mental health work is teamwork. It consists of social work, psychosocial counselling, psychotherapy and psychiatric care. Here in Seje, there’s only a social worker and a psychiatrist due to a lack of funds and trained staff. That’s all. The middle part of the pyramid, counselling and therapy, which is the most important part, is lacking completely. Proper therapy can prevent people from falling into a deep depression. Or to commit suicide. I also do therapeutic work by necessity and have a background as a therapist. But it’s not how we should work”, Dr Sadiq explains.
“Never tell women who survived ISIS and displacement and who cope with domestic violence and gender injustice, what to do. Never give advice. Never push.”
Another gap, and an aching frustration, is that, due to budget limitations, the centre in Seje does not have the psychotropic drugs patients need. Contrary to the Cordaid-supported MHPSS department in Sinjar, where all drugs, psychotropic medication included, are provided for free.
“All services in Seje are free of charge. Even antibiotics, painkillers and other essential drugs. But we lack the means to provide psychotropic drugs to treat anxiety, depression and other forms of mental suffering”, Dr Sadiq concludes. “People have to go to Dohuk for that. But the fare is too expensive for most patients, let alone the drugs.”
What we do may not be enough. It never will be. But it is essential. Sonita Khalil, Cordaid’s social worker in Seje, works at the bottom of the mental health care pyramid. Being a young Yazidi woman herself, she is a person other displaced and traumatized Yazidi women and girls can confide in. In group sessions and individual chats, in training, she creates a setting of trust and personal safety. Safe enough for girls and young women to speak out, share the pain and dream.
Watch this mini-documentary about Sonita and Cordaid’s mental health programme in Iraq:
“The first rule, as a social worker, is: never give advice”, Sonita Khalil says. “Never tell women who survived ISIS and displacement and who cope with domestic violence and gender injustice what to do. Never push. Pushing them will only cause more trouble. We can only help them to make their own choices.”
Every week, many young Yazidi women join Sonita’s ‘classes’. Most of them have been displaced for years. Moving from place to place, often in unfinished houses and never knowing how long they will be allowed to stay. Some do the vocational training, some the awareness-raising sessions, and some the reading classes. Some join all of them. When asked what Sonita offers them, her pupils in the ‘caravan’ – as they call the prefab units of the Seje health centre – shake off their reserve. “I didn’t have a clue about the menstrual cycle. Now, at least, I understand my body a bit better”, says a teenage girl. “I never finished school. Now, with Sonita, I am reading books. As a reader, I can live many lives. Non-readers can only live one life”, says 19-year-old Shamsa Matto.

“Before, I didn’t trust anyone, not even myself. Now I am not afraid anymore to trust myself”, she goes on. Nazdar Rasho, also 19, was forced to drop school after being displaced: “Sonita helps me to deal with others. And with problems.” Khaola Khedher was 13 when she fled the horrors that took place in Sinjar. “I have been displaced now for 5 years. After a few years, I left school. And now, with Sonita, I am reading books, discussing things and educating myself. It has become the most important thing in my life. It makes me happy”, she says.
Back to Sinjar
When asked whether they think of going back to Sinjar, the first answer is silence. “I’d like to”, says Khaola after a while. “But I know it will not help me. Everything is destroyed. It will never be the same again.”

Even Sonita doubts Sinjar will ever be her hometown again. She went there for the first time in five years a couple of days ago. “I was studying in the safe city of Dohuk when ISIS attacked Sinjar in 2014. My family was there. Not knowing their whereabouts and whether they had survived was horrible”, she remembers. Her family did survive. But their house was taken and damaged. And a big part of their city is in ruins. “I wanted to come here”, she says, driving through deserted and bombed streets. Some walls show black ISIS graffiti. “But I can barely look. I will never be able to live here again”, she says.
Carrying the Past While Carving a New Future
War, terror and displacement have traumatised Yazidi women beyond description. But weirdly, it has also forced them to leave their communities’ closed and often stifling settings. “Many displaced women and girls came to know a bigger world, the outside world, in the places they ended up”, Sonita says. “A world where they can wear the clothes they want. A world of social media. Places and settings where studying and working is also an option for girls. In a way, this is liberating. Look at me; I am the first girl in my extended family to have finished university studies. And even though I meet with opposition from men, I continue to set and chase my goals. While trying not to offend or estrange my family. This is what my classes and workshops are about: to help carry the suffering of what happened in the past, to carve our own future in new surroundings and to keep the bond with our families alive.”
Years after the military defeat of ISIS, Iraq – and the world – continues to grapple with what happened. The innocent are sifted from the guilty in crowded detention camps and prisons all over the country – a next-to-impossible task. Myriads of militias are inspiring security in some and fear in others. International military aircrafts keep pulling back and flying in again. European countries do whatever they can to keep their ISIS fighters inside Iraq and Syria. While all this freezes the country and catches the news, ordinary people are doing something else. They are trying to live. To move on.
By providing different types of care in different locations in and around former ISIS territory, Cordaid is strengthening a fragile health system in one of the most brutalised regions of the Middle East. In the longer run, by doing this and expanding our efforts, our people on the ground do what is needed to return to a beginning of normalcy. To help people move on.
The story was written by Frank van Lierde, corporate journalist at Cordaid.
