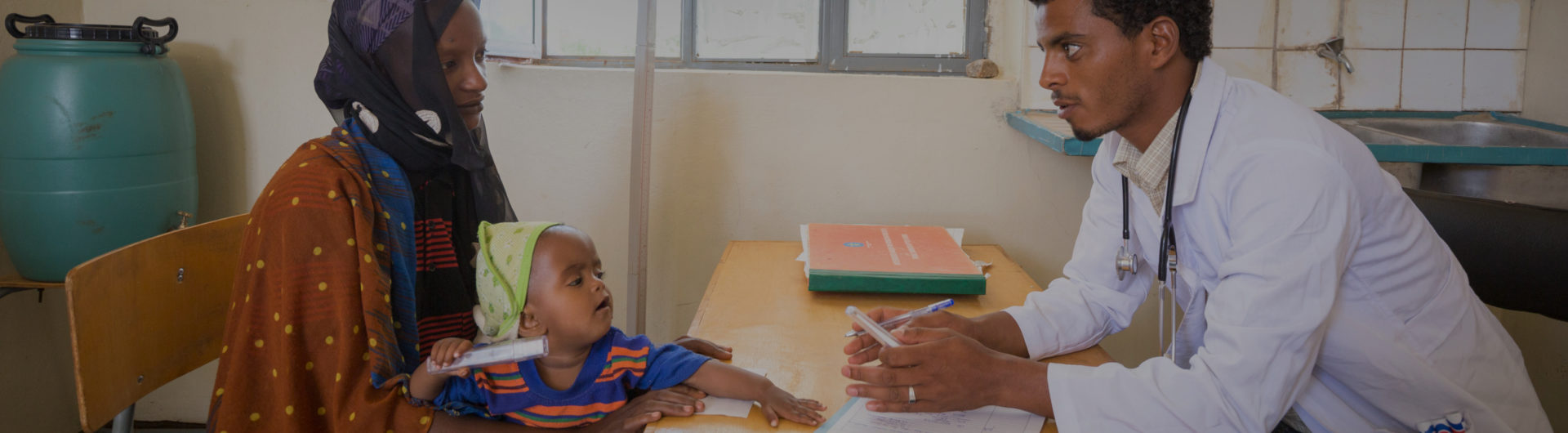
How well health facilities perform can be measured by clear indicators, for example, the quality, accessibility, and affordability of the services. In performance-based financing (PBF), health facilities get incentives based on their agreed results and can invest the obtained funds in further improving their services.
The approach also helps reform the health system to become more resilient. It starts with collaboration and a joint understanding of the pursued targets, helped by a strong monitoring system.
How PBF improves health care
PBF is a specific form of investment in health care. It can be funded either by external donors, as the Dutch government does in Ethiopia, or through domestic financing, like the Zimbabwean government allocating part of its budget through PBF. It can also be a combination of both.
Together with a purchasing agency (an independent organisation which contracts the health facilities and pays them based on their performance), the ministry of health will agree on several objectives.
Based on those objectives, specific indicators will be developed, which, when achieved, will be incentivised. For example, if the objective is to reduce the maternal mortality rate in a health clinic, one of the indicators they can agree on is the number of safe deliveries. When the agency signs a contract with a hospital or a clinic, the contract is directly based on those indicators.
Contrary to traditional funding, in PBF, health service providers such as clinics and hospitals receive incentives entirely based on their performance. The better the performance, the more bonus funds they get.
This initiates a positive cycle. The staff becomes motivated because they earn more when they offer better services, the clinic can invest in improving the facility, which helps increase the quality of the services, and as a result, the community gets better health care for an affordable price.
Results-based financing vs. performance-based financing
PBF is one form of a range of approaches which are collectively known as results-based financing (RBF). RBF covers a broad range of diverse interventions, which in one way or another all incorporate incentives or output-based payments. In the health sector, RBF is often defined as:
“Any cash payment or non-monetary transfer made to a national or sub-national government, manager, provider, payer or consumer of health services after predefined results have been attained and verified. Payment is conditional on measurable actions being undertaken.”
RBF differs from classical health financing, in the sense that it does not rely on input financing for activities to take place, but directly ties the financing of entities within the health sector to the results obtained. RBF is an approach which is increasingly being used in low- and middle-income countries to improve health system outcomes.
Performance Based Financing (PBF) is a specific form of RBF, distinguished by three conditions:
- Incentives are given to providers, not beneficiaries: the financing of health facilities is directly linked to their performance.
- Awards are purely financial; payment is by fee-for-service for specified services.
- Payments depend explicitly on the degree to which services are of approved quality, as specified by protocols for processes or outcomes.
The thread that binds it all: monitoring
As mentioned before, the ministry of health, the purchasing agency and the health facilities agree on a set of targets. The health facilities get incentives based on how far they have achieved those targets.
The question is: how is that measured and confirmed?
Three types of monitoring – or verification, as those who work with PBF call it – together do the trick. The local health authorities monitor the quality of care, whereas the purchasing agency verifies the exact number of health services delivered. The communities in their turn testify how they have perceived the quality of the services. Only after these verifications have confirmed satisfactory performance or results, the clinic or hospital gets its funding.
Thanks to the independence of the purchasing agency, conflicts of interest – which can exist in any government system when too many responsibilities are concentrated within one ministry – can be minimised. PBF improves the overall accountability of the health system. Not only by the solid monitoring mechanisms of PBF itself but also by the division of tasks among different parties.
Watch this video on how to effectively invest in health care in fragile and conflict-affected countries:
How everyone wins
Except for external and government funding, there is also a third kind of financing of health: out-of-pocket money from the patients. In many fragile countries where government and external funding for health is severely lacking, for a person, seeking health care may mean falling deeper into poverty.
And this is just the start. When people cannot afford quality health care when they need it, they cannot remain healthy, develop, and thrive. They sink deeper into poverty and misery. As individuals and as a country. Limited or no access to health care starts the cycle of less productivity, fewer taxes, and thus less government funding for health.
With PBF, the investment in health creates a positive ripple. It makes good quality health care affordable and available. This will result in a healthier population, able to help the country progress and prosper.
PBF works! We just need to make it happen
Some African countries are implementing PBF with success. Cordaid has been part of some of these success stories, for instance in Rwanda, Zimbabwe and Ethiopia.
PBF means being wise about every penny invested in health in fragile countries. And the reward we harvest is a healthcare system that is strong and can go a long way in providing essential health services. Now, more investment through PBF is needed in health. For greater results, and to start the positive cycle of health and prosperity.